FirstName LastName’s Poster
Title Case
by Runqin Shi1,2,3, Jimmy Pengyu Chen1,2, Jade Wei1,2, Talia Rosen3, Laura Baruch3, & Sarah Bloch-Elkouby1,3
1 Icahn School of Medicine at Mount Sinai in New York City
2 Teachers College, Columbia University in the City of New York
3 Ferkauf Graduate School of Psychology, Yeshiva University

Background:
- Despite increased awareness of racial disparities in healthcare, implicit racial biases continue to persist and influence clinical practice (Charlesworth & Banaji, 2019).
- While explicit racial biases among Americans declined by 37% between 2007 and 2016, implicit biases decreased by only 17%, indicating that many individuals may still hold unconscious prejudices they are unaware of or unwilling to report (Charlesworth & Banaji, 2019).
- Implicit racial biases have been shown to negatively impact clinical decisions, weaken therapeutic alliances, and contribute to poorer treatment outcomes for racially minoritized patients (Maina et al., 2018; Penner et al., 2014).
- Few studies examined how implicit racial biases influence professionals’ interactions with Black adolescents, a group disproportionately affected by suicide risk and systemic inequities in mental healthcare compared to their White peers (Lindsey et al., 2019; Nestor et al., 2016).
Objective:
- To address these critical gaps in the literature, the current study uses Virtual Human Interaction (VHI) technology to simulate realistic clinical encounters (Rossen et al., 2008) and is therefore well suited to examine how implicit racial biases influence clinicians’ engagement and enjoyment in interactions with racially diverse adolescent patients.
- The current study examined whether virtual patients’ race and clinicians’ implicit racial biases impact clinicians’ interaction time and their enjoyment of clinical interviews with Black vs. White virtual patients, and whether the results are moderated by clinicians’ race.
- We hypothesized that clinicians would conduct a shorter interview and report lower enjoyment with black virtual patients compared to white patients. We also hypothesized that clinicians with higher levels of implicit racial bias would be associated with shorter clinical interviews and lower enjoyment.
- We did not hypothesize the moderate effect of clinicians’ races due to the lack of prior work.
Method:
Participant
Participants (N=138, M=28.74, SD=3.57, range: 22-48 years old) are licensed and pre-licensed mental health professionals recruited from clinical psychology programs around the U.S. They were randomly assigned to interact with a Virtual Patient of either race.
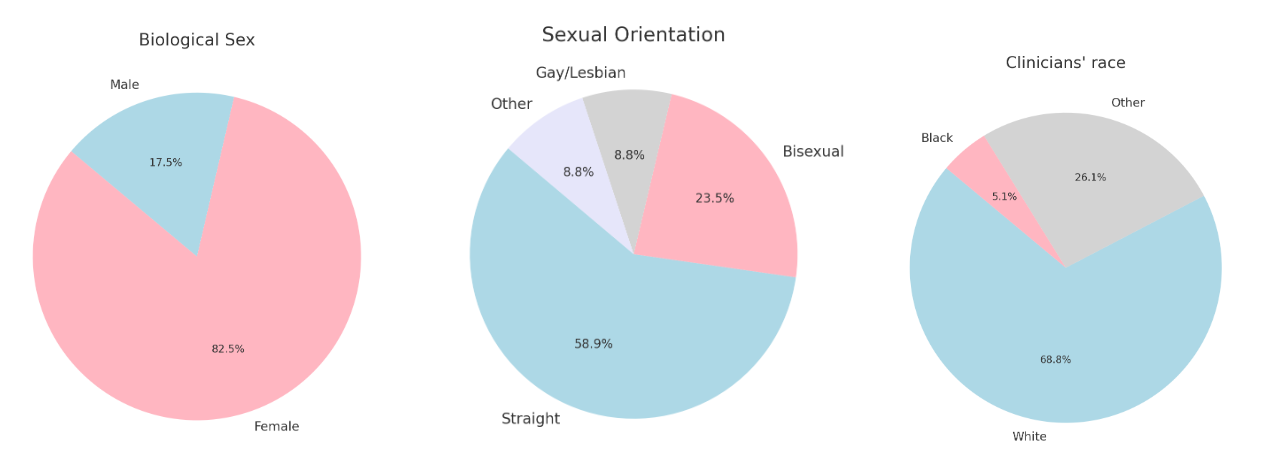
Measures
- Implicit racial biases were measured using the Race Implicit Association Test (IAT; Greenwald, Nosek, & Banaji, 2003). 3 categories: high white preference (-3, -2), neutral (-1, 0, 1), and high black preference (2, 3)
- Interaction length was timed in minutes by the VHI system
- Clinicians’ enjoyment of the interaction was self-reported using a 1-item5-point Likert scale (1 = Poor, 5 = Excellent)
- Clinicians’ racial identity, the moderator, was self-reported and categorized into White, Black, and Other
Statistical Analyses
- Preliminary analyses involved reporting descriptive statistics and intercorrelations between demographics, implicit biases, interaction length, and enjoyment outcome.
- Primary analyses utilized two linear regression models to test effects of virtual patients’ race and clinicians’ implicit biases and their interaction with clinicians’ self-identified race, with the following study outcome variables: clinicians’ interaction time and their enjoyment of clinical interviews. Covariates included clinician age, biological sex, and sexual orientation.
- Given the substantial imbalance in clinician race (White: n=95; Other: n=36; Black: n=7), we applied bootstrap resampling with replacement to balance group sizes and reduce bias in estimating interaction effects. Each racial group was resampled to match the size of the largest group (n=95), resulting in a synthetic balanced dataset. Analyses were conducted using this balanced dataset to improve the reliability of comparisons across clinician racial identity.
- Sensitivity analyses using the original (unbalanced) dataset were also conducted to assess the robustness of findings.
- Model 1 examined the effects of patient race and clinician implicit bias (IAT) on interaction length, with clinician race as a moderator.
- Model 2 examined the effects of patient race and clinician implicit bias (IAT) on enjoyment of the interaction, with clinician race as a moderator.
Results:
- Two regression analyses were conducted with two outcomes (interaction length: Adjusted R-squared=0.401, p<.0001; enjoyment: Adjusted R-squared=0.156, p<.0001).
- There is no indication that the race of the virtual patient alone affects interaction length.
- Neutral implicit racial bias predicts longer sessions overall compared to high White or Black preference; except for White clinicians, where neutral bias predicts shorter sessions overall; meanwhile, White clinicians with neutral bias reported higher enjoyment, compared to those with Black preference bias.
- White clinicians (vs. Black clinicians) spent significantly more time with virtual patients, regardless of virtual patient race.
- Clinicians reported greater enjoyment with White virtual patients. But this is moderated by clinician race: non-White clinicians reported lower enjoyment in White-patient interactions.
- Sensitivity Analysis: When the same models were run using the original (unbalanced) dataset, key effects were no longer statistically significant. This likely reflects limited power due to small sample sizes in underrepresented clinician groups. These results highlight the need for larger, more diverse samples to robustly detect interaction effects.
Discussion:
- The sample is skewed toward young, female, and White clinicians, which limits generalizability. Future studies can include more black and male clinicians with a wider age range to balance groups and increase power for racial interaction effects and overall validity.
- We may explore how other factors, such as technical issues, therapeutic alliance measures, and the length of clinicians’ training, affect or moderate the study outcomes.
- This study provides valuable exploratory evidence about how clinicians’ implicit racial biases and their own racial identities can influence the length and their enjoyment of their clinical interaction, which are critical components of effective mental health care.
References:
Charlesworth, T. E. S., & Banaji, M. R. (2019). Patterns of implicit and explicit attitudes: I. Long-term change and stability from 2007 to 2016. Psychological Science, 30(2), 174–192. https://doi.org/10.1177/0956797618813087
Greenwald, A. G., Nosek, B. A., & Banaji, M. R. (2003). Understanding and using the implicit association test: I. An improved scoring algorithm. Journal of Personality and Social Psychology, 85(2), 197–216. https://doi.org/10.1037/0022-3514.85.2.197
Lindsey, M. A., Sheftall, A. H., Xiao, Y., & Joe, S. (2019). Trends of suicidal behaviors among high school students in the United States: 1991–2017. Pediatrics, 144(5). https://doi.org/10.1542/peds.2019-1187
Maina, I. W., Belton, T. D., Ginzberg, S., Singh, A., & Johnson, T. J. (2018). A decade of studying implicit racial/ethnic bias in healthcare providers using the implicit association test. Social Science & Medicine, 199, 219–229. https://doi.org/10.1016/j.socscimed.2017.05.009
Nestor, B. A., Cheek, S. M., & Liu, R. T. (2016). Ethnic and racial differences in mental health service utilization for suicidal ideation and behavior in a nationally representative sample of adolescents. Journal of Affective Disorders, 202, 197–202. https://doi.org/10.1016/j.jad.2016.05.021
Penner, L. A., Blair, I. V., Albrecht, T. L., & Dovidio, J. F. (2014). Reducing racial health care disparities: A social psychological analysis. Policy Insights from the Behavioral and Brain Sciences, 1(1), 204–212. https://doi.org/10.1177/2372732214548430
Rossen, B., Johnsen, K., Deladisma, A., Lind, S., & Lok, B. (2008). Virtual humans elicit skin-tone bias consistent with real-world skin-tone biases. In Intelligent Virtual Agents: 8th International Conference, IVA 2008, Tokyo, Japan, September 1–3, 2008. Proceedings (pp. 237–244). Springer Berlin Heidelberg. https://doi.org/10.1007/978-3-540-85483-8_24