Jade Wei’s Poster
Does Mindfulness Moderate the Impact of Patients’ Race and Clinicians’ Implicit Racial Biases on Clinicians’ Emotional Response to Minoritized Youth?
by Jade Wei1,2, Runqin Shi1,2,3, Jimmy P. Chen1,2, Wendy Guo1,2, Jason Tortora3, & Sarah Bloch-Elkouby2,3
1 Teachers College, Columbia University in the City of New York
2 Icahn School of Medicine at Mount Sinai in New York City
3 Ferkauf Graduate School of Psychology, Yeshiva University

Background:
- Provider bias may contribute to persistent disparities in mental health service utilization.
- The impact of provider bias on clinicians’ emotional responses in therapy is not well understood.
- The potential protective role of clinicians’ mindfulness in this context has not been explored.
- This study examines:
- How patients’ race and clinicians’ implicit racial bias affect clinicians’ emotional responses.
- Whether clinicians’ mindfulness moderates these effects.
Objective:
- Clinicians would show significantly different emotional responses to virtual patients of different races.
- There will be an interaction effect between virtual patients’ race and clinicians’ implicit racial biases, on the one hand, and clinicians’ emotional response to the virtual patients, such that clinicians with a higher implicit racial biases level will report more negative emotional responses to Black vs. White virtual patients.
- The level of clinicians’ mindfulness will moderate the relationship between virtual patients’ race and clinicians’ implicit racial biases, and clinicians’ emotional response, such that among clinicians with a higher level of mindfulness, the relationship between our virtual patients’ race and clinicians’ implicit racial biases, and clinicians’ emotional response will be weaker.
Method:
Participants: 200 mental health professionals.
Design: Randomized assignment to virtual patients (Black vs. White).
Procedure: Clinicians conducted simulated clinical interviews.
Measures:
- Emotional response: Therapist Response Questionnaire- Short Form (TRQ-SF)
- Mindfulness: Mindful Attention Awareness Scale (MAAS)
- Implicit bias: Implicit Association Test (IAT)
Analysis: Independent t-test and PROCESS macro (Models 1 & 3) to test moderation and three-way interaction effects.
Results:
-
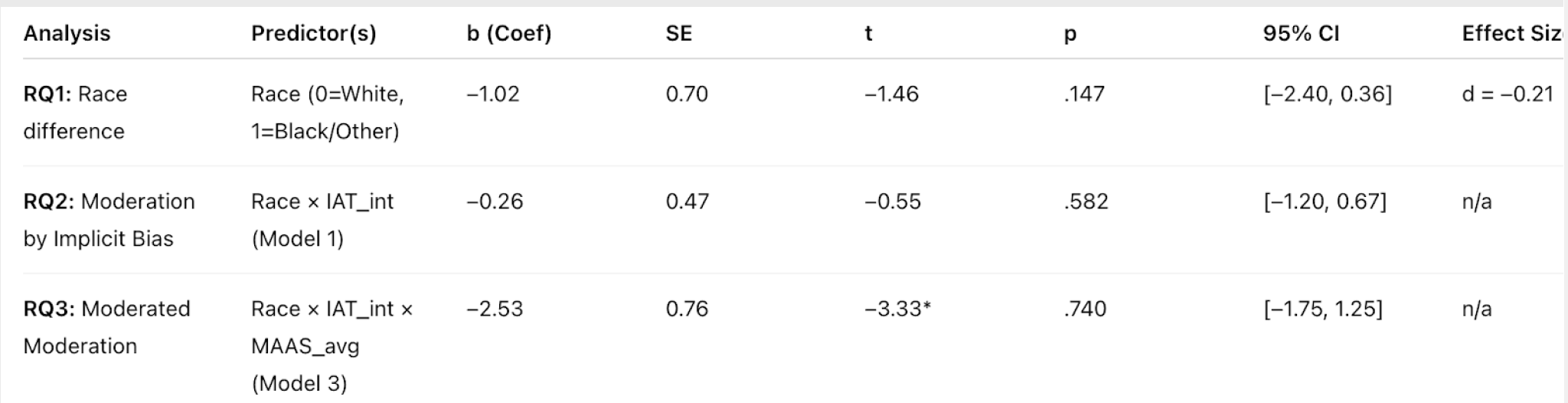
Race difference (RQ1): There was no significant difference in clinicians’ emotional responses between those assigned to White (M=17.19, SD=4.74, n=100) and Black/Other (M=18.21, SD=4.91, n=91) virtual patients, t(185.9) = -1.46, p = .147, 95% CI [-2.40, 0.36]. The effect size was small, d = –0.21, 95% CI [–0.50, 0.07].
-
Moderation by implicit bias (RQ2): The interaction between patient race (group) and implicit racial bias (IAT_int) was not significant, b = –0.26, SE = 0.47, t = –0.55, p = .58, 95% CI [–1.20, 0.67], indicating clinicians’ implicit bias did not moderate the effect of patient race on emotional response.
-
Three-way interaction (RQ3): The three-way interaction between patient race, implicit bias, and mindfulness was also not significant, b = –2.53, SE = 0.76, t = –3.33, p = .74, 95% CI [–1.75, 1.25]. There was no evidence that mindfulness further moderated the effect of race and implicit bias on clinicians’ emotional responses.
Discussion:
RQ1: In this virtual simulation, clinicians’ emotional responses did not differ noticeably based on the virtual patient’s race. It is unclear whether this reflects the influence of the virtual platform or an absence of negative responses; other factors, such as the virtual patient’s facial expressions or head movements, may also have played a role.
RQ2: No significant interaction was observed between patient race and clinicians’ implicit racial bias. This suggests that, in this context, higher implicit bias did not meaningfully affect clinicians’ emotional responses by race. Future studies may consider alternative measures or methods to assess bias.
RQ3: Mindfulness did not further moderate the relationship between race, bias, and emotional response. This may relate to the specific mindfulness measure used or the simulation context.
Conclusion:
The present study explored how patient race, clinicians’ implicit racial bias, and mindfulness might shape clinicians’ emotional responses within a virtual clinical context. While patterns of response did not align with our initial hypotheses, the findings offer important insights into the complexity of interpersonal processes in simulated settings. The absence of strong effects in this sample may reflect the influence of additional contextual factors, or suggest that virtual patient paradigms capture only certain dimensions of clinician experience. These results highlight the value of continued research using diverse methodologies to better understand how bias and mindfulness may influence clinical interactions across settings.
Limitation:
The use of virtual patients may not fully capture the complexity of real clinical interactions. Self-report measures can be influenced by social desirability or limited self-insight. The sample may not represent all mental health professionals, and the cross-sectional design limits causal interpretations. The study may also have lacked power to detect small effects, and unmeasured variables may have influenced results.
References:
Betan, E., Heim, A. K., Zittel Conklin, C., & Westen, D. (2005). Countertransference phenomena and personality pathology in clinical practice: An empirical investigation. American Journal of Psychiatry, 162(5), 890–898. https://doi.org/10.1176/appi.ajp.162.5.890
Brown, K. W., & Ryan, R. M. (2003). The benefits of being present: Mindfulness and its role in psychological well-being. Journal of Personality and Social Psychology, 84(4), 822–848. https://doi.org/10.1037/0022-3514.84.4.822
Brown, K. W., West, A. M., Loverich, T. M., & Biegel, G. M. (2011). Assessing adolescent mindfulness: Validation of an adapted Mindful Attention Awareness Scale in adolescent normative and psychiatric populations. Psychological Assessment, 23(4), 1023–1033. https://doi.org/10.1037/a0021338
Greenwald, A. G., Nosek, B. A., & Banaji, M. R. (2003). Understanding and using the Implicit Association Test: I. An improved scoring algorithm. Journal of Personality and Social Psychology, 85(2), 197–216. https://doi.org/10.1037/0022-3514.85.2.197
Zittel Conklin, C., & Westen, D. (2003). The Therapist Response Questionnaire. Departments of Psychology and Psychiatry and Behavioral Sciences, Emory University, Atlanta, GA.